Aesthetic Dermatology
Skin Diseases in Adults
Vitiligo
Vitiligo is an acquired disorder of the skin and mucous membranes characterized by well-demarcated depigmented (white) macules and patches. Its worldwide prevalence ranges from 0.5% to 2% of the general population.
The exact mechanism leading to melanocyte destruction and disappearance in affected skin has not been fully elucidated. Several pathogenetic theories have been proposed; for non-segmental vitiligo, the most widely accepted is the autoimmune hypothesis.
Based on the distribution and extent of lesions, vitiligo is classified as localized, generalized, and universal. The disease typically progresses slowly; however, it may remain stable for long periods or worsen abruptly.
Treatment options include:

- Topical therapy
- Phototherapy
- Laser therapy
- Surgical interventions
- Depigmentation of uninvolved (normal) ski
Response to treatment depends primarily on lesion location and the patient’s Fitzpatrick skin phototype. Relapses are common.
Atopic Dermatitis / Eczema / Xerosis
A chronic, relapsing, pruritic inflammatory dermatosis with a hereditary predisposition, affecting 5%–20% of children and 0.9%–3% of adults. Therapeutic management depends on disease severity; however, even during remission, maintenance measures and avoidance of triggering and aggravating factors are essential.
It is the most common chronic dermatosis in children. In 80% of cases, onset occurs before the age of five, although in recent years adult-onset atopic dermatitis has increased. Approximately 50% of cases improve by preschool age, and 75%–80% show improvement or remission by preadolescence.
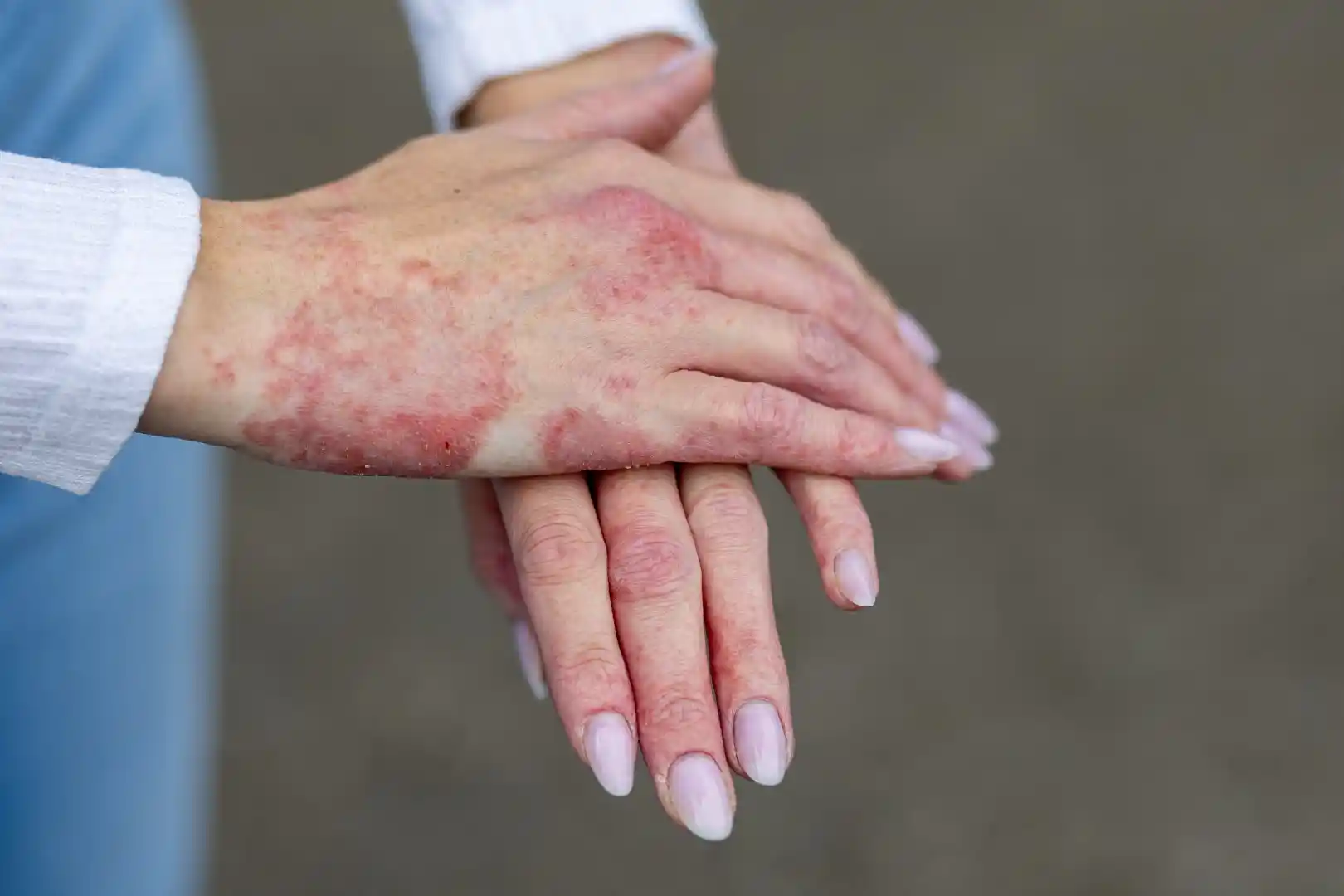
In 30%–50% of patients, allergic bronchial asthma and/or allergic rhinitis may develop later in life, depending on the severity of atopic dermatitis. In 10%–20%, the disease persists lifelong.
Scabies
A highly contagious parasitic dermatosis. The hallmark symptom is intense nocturnal pruritus. Clinical variants that may escape suspicion include infantile scabies and “Norwegian” (crusted) scabies.
Delayed diagnosis contributes to outbreaks, particularly in schools, hospitals, and long-term care facilities.
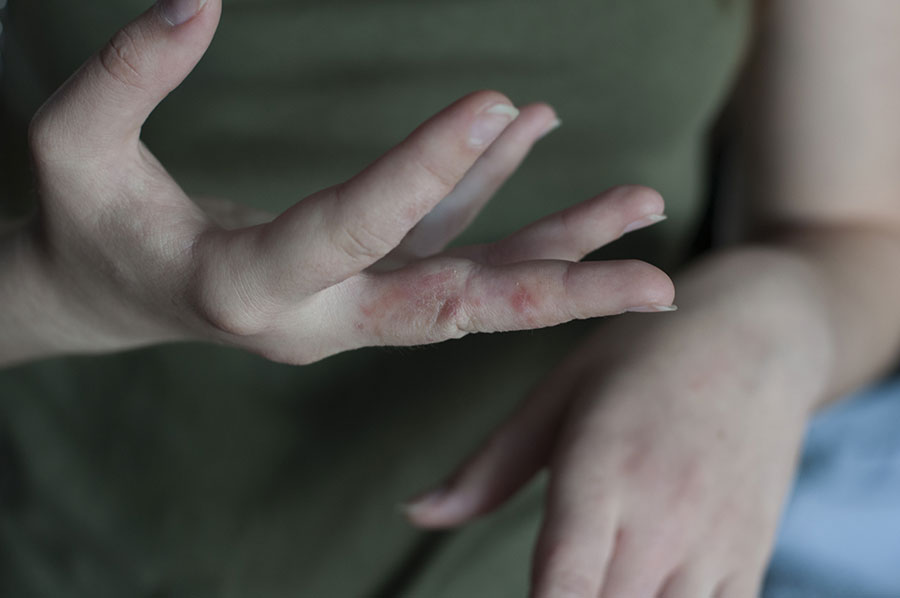
Meticulous application of antiparasitic agents, treatment repetition when indicated, simultaneous treatment of close contacts, and disinfection of clothing and bedding are essential prerequisites for successful management.
Psoriasis
Psoriasis is a chronic, non-contagious, inflammatory dermatosis characterized by abnormal proliferation and differentiation of keratinocytes, leading to the development of typical psoriatic lesions. It is common, affecting approximately 1.5%–3% of the global population. It occurs at all ages and affects both sexes equally. About two-thirds of patients have mild disease and one-third have moderate-to-severe disease.
Its onset is attributed to environmental triggering factors acting on genetically predisposed individuals, resulting in a distinctive immune-mediated response. Triggers include trauma, infections, medications, sunlight, metabolic factors, hormonal factors, stress, alcohol, and smoking.
Chronic plaque psoriasis is the most common form. Other forms include:
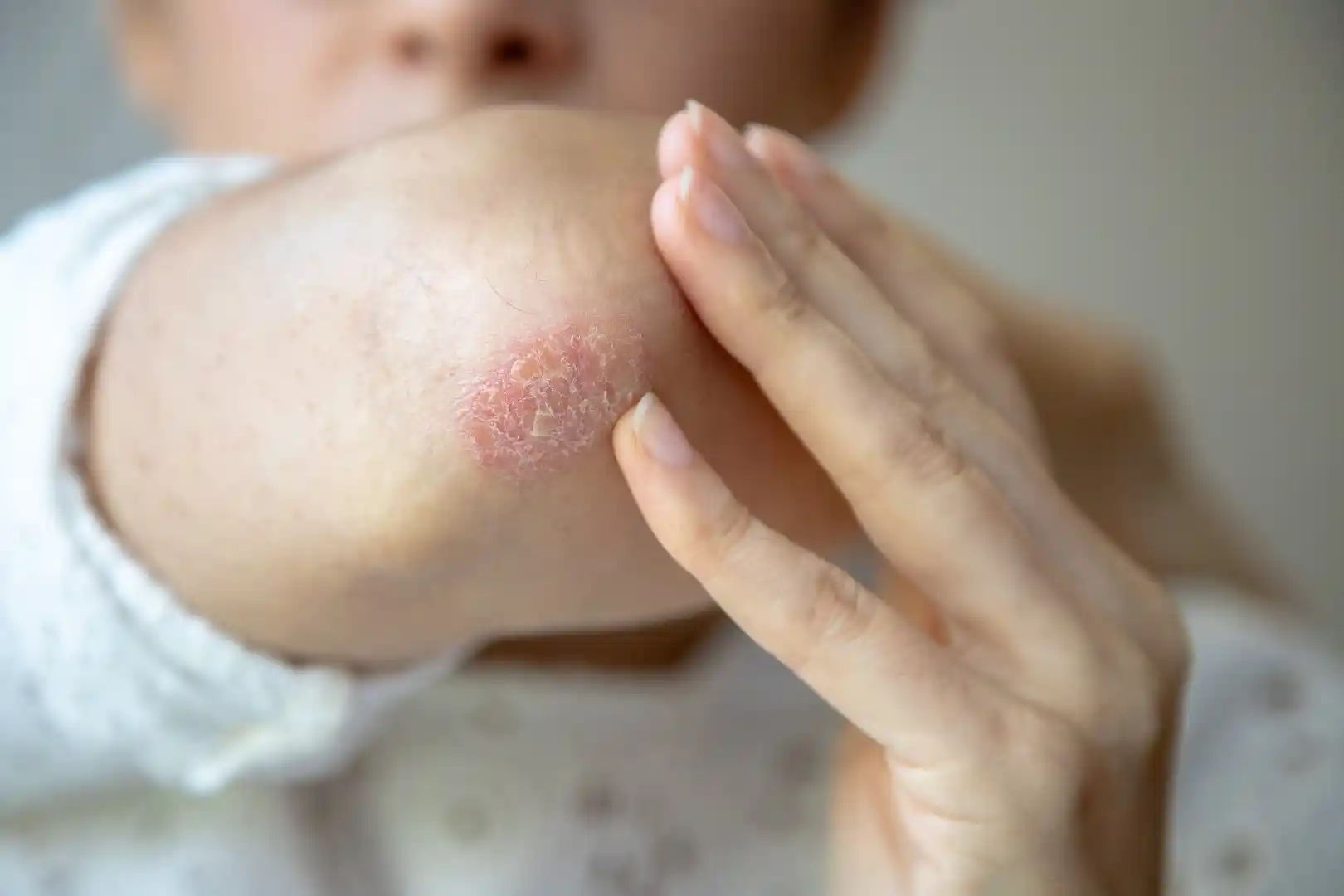
- Guttate
- Erythrodermic
- Pustular psoriasis
- Psoriasis may involve the scalp
- Palms and soles
- Genital and mucosal surfaces
- Nails (nail psoriasis)
- Inverse psoriasis
- Psoriatic onychodystrophy
Treatment is individualized according to extent, severity, and patient-specific factors, and includes topical therapy, systemic therapy, and phototherapy.
Urticaria
Acute and chronic urticaria are common syndromes triggered by a wide range of factors. Urticaria is classified as spontaneous (acute or chronic), physical urticaria (cold, delayed pressure, heat, solar), factitious urticaria/dermographism, vibratory angioedema, and other forms (aquagenic, cholinergic, contact, exercise-induced).
The mast cell is the key cell in urticaria pathogenesis. Mast-cell degranulation may occur via:
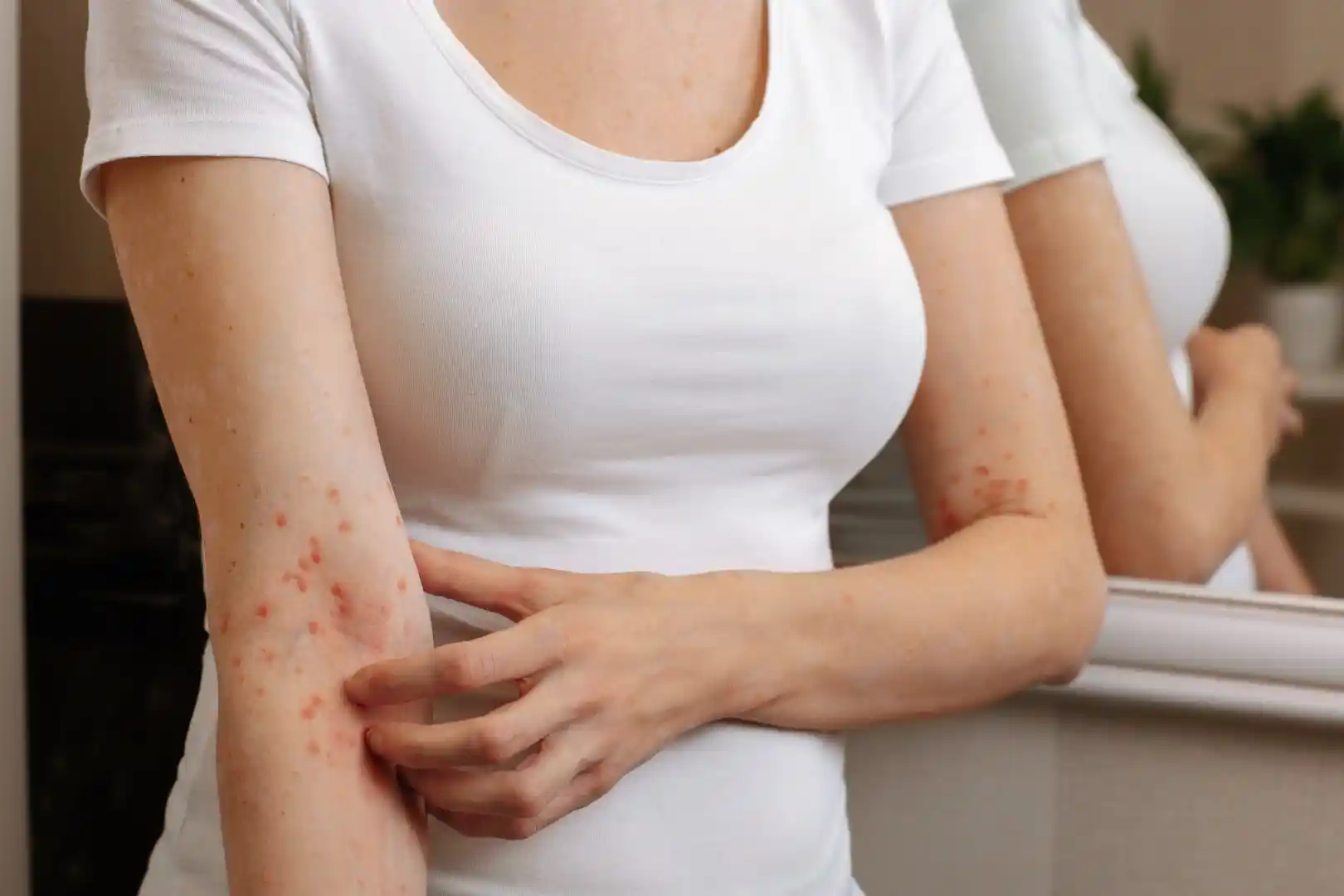
- IgE-dependent mechanisms
- Complement-dependent mechanisms
- IgG autoantibody-mediated mechanisms
- Non-immunologic mechanisms
Because etiologies are numerous, identification and avoidance/discontinuation of the causative factor (medications, foods, infections, etc.) is central to management. H1-antihistamines—primarily second-generation—are first-line therapy. Systemic corticosteroids, cyclosporine, dietary measures, and stress avoidance may be recommended in selected cases.
Adult Acne (Cystic Acne and Rosacea)
Acne is a dermatosis resulting from internal and/or external factors. It most commonly affects adolescents due to the onset of androgen production, which regulates sebaceous gland activity and sebum secretion; among internal factors, heredity is particularly important.
External contributors include high environmental humidity, certain medications, exposure to chemicals, and inappropriate cosmetic products.
Three main pathogenetic disturbances lead to acne:

- Seborrhea (increased sebum production)
- Follicular hyperkeratinization with obstruction of pilosebaceous ducts and subsequent overgrowth of skin-resident microbes (primarily Cutibacterium acnes, formerly Propionibacterium acnes)
- Inflammation
Clinically, increased skin oiliness and open or closed comedones (blackheads or whiteheads) are seen initially. Later, inflammatory lesions develop: papules and pustules; in more severe disease, painful deep nodules or cysts.
According to predominant lesions, acne is classified as comedonal, papulopustular, or nodulocystic, and graded as mild, moderate, or severe based on lesion count. Acne may affect not only the face but also the décolleté, back, shoulders, and neck.
In recent years, post-adolescent (adult) acne—particularly in women—has become more common, with hormonal factors and modern lifestyle influences implicated (stress, environmental pollution, poor diet, excessive or unsuitable cosmetic use).
Premenstrual flares are also frequent. Early diagnosis is important, especially when scarring is a concern, and dermatologic evaluation is recommended for appropriate individualized treatment.
Fungal Infections (Mycoses)
Dermatophytes selectively infect keratinized tissues (skin and nails). Prompt treatment is required to prevent spread and transmission.
Common oral antifungals include:

- Itraconazole
- Fluconazole
- Terbinafine
- Griseofulvin
Candida albicans is the principal causative agent of candidiasis. Predisposing factors include age, pregnancy, immunosuppression, maceration, dentures, occlusion, antibiotic use, iron deficiency, and hormonal disturbances.
Pityriasis versicolor is a chronic, superficial, relapsing, and often asymptomatic infection of the stratum corneum caused by Malassezia yeasts. Early diagnosis and treatment with topical or systemic antifungal agents are required.
Hyperhidrosis
Hyperhidrosis is the medical term for excessive sweating beyond physiological needs. It may occur year-round and can be influenced by emotional stimuli. Summer heat can significantly affect quality of life.

Botulinum toxin injections are a highly effective therapeutic option that can markedly improve daily functioning.
Melasma
Melasma is a common acquired disorder of hyperpigmentation. It typically presents as symmetrical, irregular macules and patches ranging from light gray to dark brown.
It occurs on sun-exposed areas, mainly the face. It predominantly affects women with darker skin types, during adolescence or later in life. Although its exact pathogenesis is unknown, ultraviolet radiation is considered the most important etiologic factor.

Treatment should be individualized according to melasma type and patient characteristics, and combination therapies often yield better outcomes. Avoidance of aggravating factors and counseling regarding the chronic nature of the condition and the need for maintenance therapy are essential.
Drug Eruptions
Cutaneous drug reactions are the most common type of adverse drug reaction in both adults and children. Most are caused by antibiotics, particularly penicillins and cephalosporins.
Drug eruptions can clinically mimic virtually any dermatosis. The most common presentations are exanthematous (morbilliform or maculopapular) eruptions (75%–95%) and urticaria (5%–6%). Management focuses on discontinuation of the offending medication.

Symptomatic therapy with antipruritic agents and topical corticosteroids may be helpful. Any rash occurring within two weeks of starting a medication should include “drug eruption” in the differential diagnosis.
Herpes Simplex
Herpes simplex infections are caused by HSV-1 and HSV-2, responsible primarily for herpes labialis and genital herpes, respectively.

Recurrent herpes simplex most often appears on the lips, at least 3–4 times annually, as vesicles that crust within 3–4 days and resolve within 8–9 days without scarring.
Herpes Zoster
Varicella-zoster virus (VZV) causes chickenpox and herpes zoster. Chickenpox results from primary infection, whereas herpes zoster represents reactivation of latent infection.
Prodromal symptoms preceding the rash include:
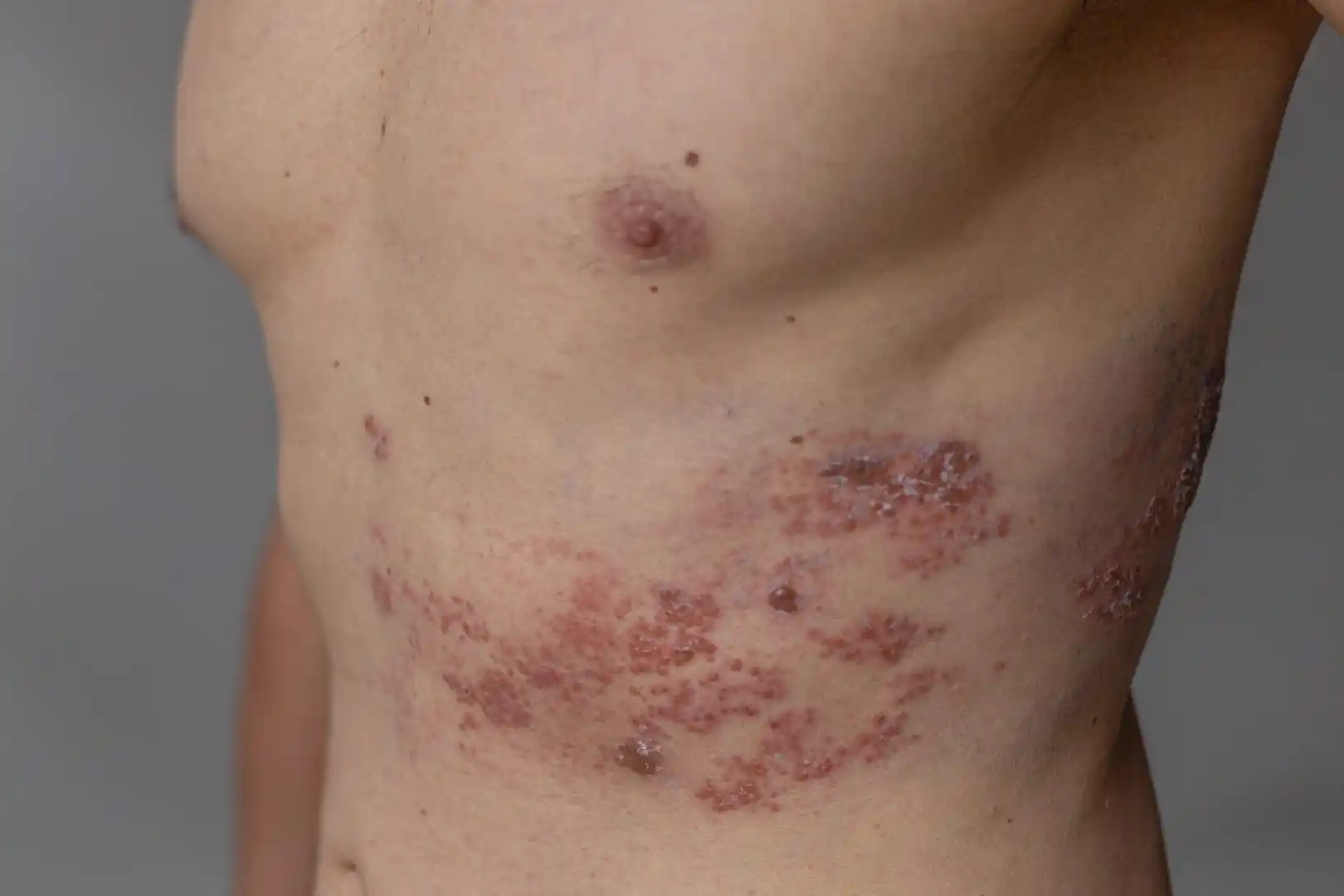
- Localized pain
- Burning
- Pruritus
- Hyperesthesia in the affected dermatome in more than 90% of cases.
